3 results
High prevalence of antibiotic use in a tertiary-care hospital in Sierra Leone: We need to handle antibiotics with care
- Ibrahim Franklyn Kamara, Bobson Fofanah, Bockarie Pharaj Sheriff, Victoria Katawera, Robert Musoke, Sulaiman Lakoh, Kadijatu Nabie Kamara, Joseph Sam Kanu
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s22-s23
-
- Article
-
- You have access Access
- Open access
- Export citation
-
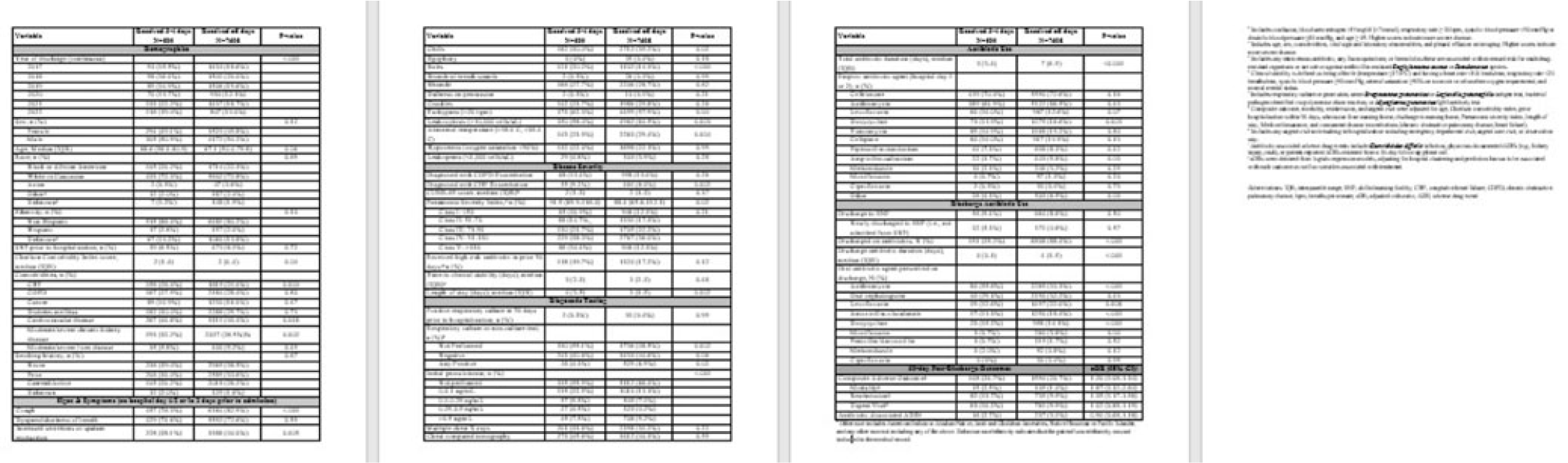
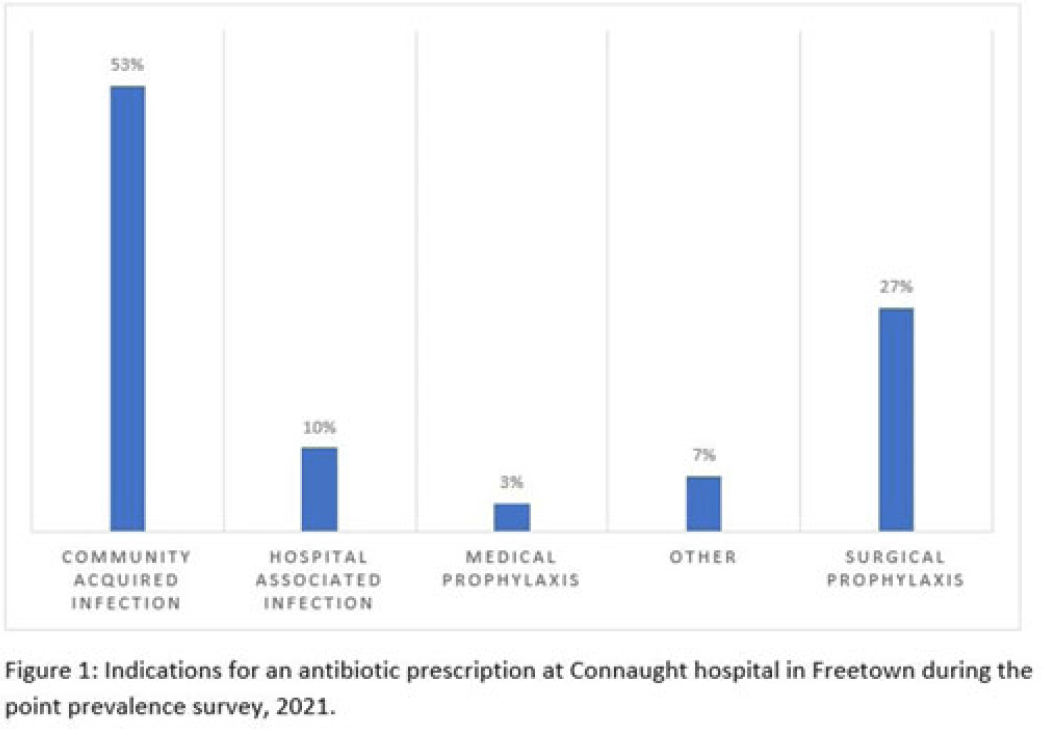
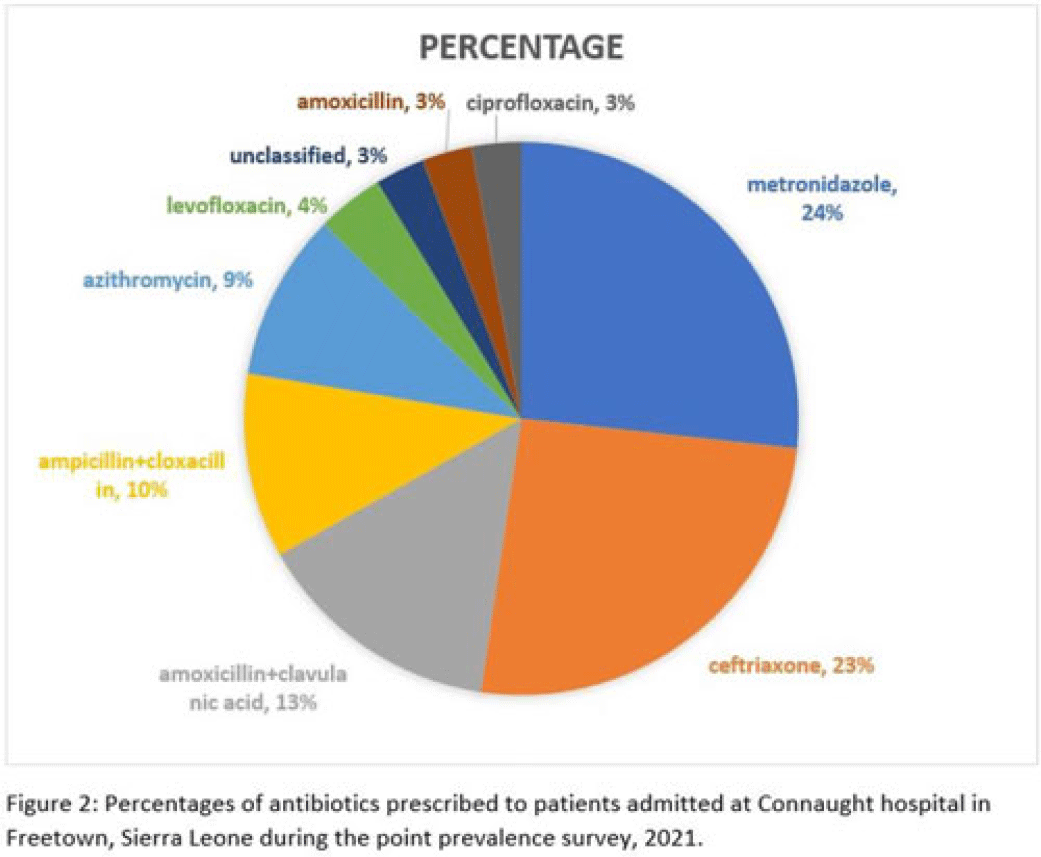
Background: Antimicrobial resistance (AMR) is a global public health concern that has the potential to reverse decades of progress aimed at decreasing morbidity and mortality attributed to infectious diseases. In 2019, ~5 million deaths were associated with AMR, of which 1.2 million were attributed to antibacterial-resistant infections. Healthcare facilities where antimicrobials are frequently used are high-risk settings for the selection and spread of resistant bacteria, and they further contribute to the increase in the burden of AMR. We have documented the prevalence and indication of antibiotic use in a tertiary-care referral hospital in Freetown, Sierra Leone. Methods: This point-prevalence survey was conducted at Connaught hospital, a tertiary-care hospital in Sierra Leone, in November 2021. The hospital offers a range of medical and surgical services through 25 units and has 16 wards with >300 beds. Data on patient-level antibiotic use, including indications for use, were extracted from medical records using WHO point-prevalence survey (PPS) forms that had been pretested and validated. Data collection was conducted in all the wards over a 10-day period by trained healthcare personnel. On the day of the survey, only the medical records of patients on admission before 8:00 a.m. on that day were included in the study. Data entry, cleaning, and analysis were conducted using the WHO PPS platform. Ethical approval was obtained. Results: In total, 87 patient records were included in the survey. Most (71%) were women, and the average age was 30.6 years. The prevalence of antibiotic use was 66%, and the average number of antibiotics prescribed to patients since admission was 2. The 5 most prescribed antibiotics were metronidazole, ceftriaxone, amoxicillin and clavulanic acid, ampicillin and cloxacillin, and azithromycin. The parenteral route of drug administration was the mainstay. The most frequent indications for antibiotic prescription were community-acquired infection and surgical prophylaxis. Blood-culture requests were not ordered before the initiation of antibiotic treatment. Conclusions: This study was the first study to be conducted in Connaught hospital using the WHO PPS methodology. The survey reports a high prevalence (60%) of antibiotic use, and most treatment was done empirically. This finding is contrary to the WHO recommendation of <30% antibiotic use. This high prevalence of antibiotic use has the potential to increase the burden of AMR in the country. Therefore, there is an urgent need to strengthen Connaught hospital’s antibiotic stewardship program.
Disclosures: None
High levels of surgical antibiotic prophylaxis: Implications for hospital-based antibiotic stewardship in Sierra Leone
- Sulaiman Lakoh, Joseph Sam Kanu, Sarah K. Conteh, James B.W. Russell, Stephen Sevalie, Christine Ellen Elleanor Williams, Umu Barrie, Aminata Kadie Kabia, Fatmata Conteh, Mohamed Boie Jalloh, Gibrilla F. Deen, Mustapha S. Kabba, Aiah Lebbie, Ibrahim Franklyn Kamara, Bobson Derrick Fofanah, Anna Maruta, Christiana Kallon, Foday Sahr, Mohamed Samai, Olukemi Adekanmbi, Le Yi, Xuejun Guo, Rugiatu Z. Kamara, Darlinda F. Jiba, Joseph Chukwudi Okeibunor, George A. Yendewa, Emmanuel Firima
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 07 July 2022, e111
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Despite the impact of inappropriate prescribing on antibiotic resistance, data on surgical antibiotic prophylaxis in sub-Saharan Africa are limited. In this study, we evaluated antibiotic use and consumption in surgical prophylaxis in 4 hospitals located in 2 geographic regions of Sierra Leone.
Methods:We used a prospective cohort design to collect data from surgical patients aged 18 years or older between February and October 2021. Data were analyzed using Stata version 16 software.
Results:Of the 753 surgical patients, 439 (58.3%) were females, and 723 (96%) had received at least 1 dose of antibiotics. Only 410 (54.4%) patients had indications for surgical antibiotic prophylaxis consistent with local guidelines. Factors associated with preoperative antibiotic prophylaxis were the type of surgery, wound class, and consistency of surgical antibiotic prophylaxis with local guidelines. Postoperatively, type of surgery, wound class, and consistency of antibiotic use with local guidelines were important factors associated with antibiotic use. Of the 2,482 doses administered, 1,410 (56.8%) were given postoperatively. Preoperative and intraoperative antibiotic use was reported in 645 (26%) and 427 (17.2%) cases, respectively. The most commonly used antibiotic was ceftriaxone 949 (38.2%) with a consumption of 41.6 defined daily doses (DDD) per 100 bed days. Overall, antibiotic consumption was 117.9 DDD per 100 bed days. The Access antibiotics had 72.7 DDD per 100 bed days (61.7%).
Conclusions:We report a high rate of antibiotic consumption for surgical prophylaxis, most of which was not based on local guidelines. To address this growing threat, urgent action is needed to reduce irrational antibiotic prescribing for surgical prophylaxis.
Point-Prevalence Survey on Antibiotics Use in Six Regional Hospitals in Sierra Leone
- Ralph Williams, Christiana Conteh, Joseph Sam Kanu
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s494
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: Antibiotic resistance (AMR) is a safety concern for patients in Sierra Leone. AMR can occur in communities and as well in the process of receiving treatments in healthcare settings, and it can pose a major threat to patient safety. Healthcare-associated infections and AMR result in longer duration of illness, longer treatment, higher mortality, increased costs, and increased burden to health facilities. Objective: The purpose of this study was to generate more reliable estimates of the risk factors for the prevalence of HAI and to investigate patterns of antibiotic prescriptions done. Methods: The survey was conducted in 6 regional hospitals in Sierra Leone (Kono, Kambia, BO, Makeni, Moyamba, and Kenema) from June 16 to July 10 2019. The survey targeted inpatients in the pediatric, maternity, medical, and surgical wards. A structured questionnaire adopted from the WHO PPS form was used to collect information from patient medical charts and care notes. Results: Data were collected from 156 patients, of whom 140 patients were on antibiotics, 100 were women, and 40 were men. Patients on 1 antibiotic regimen accounted for 8.6% (n = 12) and 91.4% (n = 128) on a regimen of 2 or 3 antibiotics. Only 5 patients (3.6%) were on oral antibiotics and 135 (96.4%) were on IV antibiotics. In the maternity ward, 28 of 40 patients (70%) had had a caesarian section and were on 2 or more antibiotics; 18 patients with caesarian sections (64.3%) developed complications and continued on an antibiotic regimen for >1 week. The remaining 12 patients (30%) in the maternity ward were admitted for anemia and hypertension (ie, preeclampsia), and these patients were on 1 antibiotic regimen for which they had no clinical indication. Conclusions: The survey results show that every patient admitted to the hospital was covered with antibiotics with or without indications; no laboratory investigations were performed before antibiotics were initiated. These findings further reveal a large number of patients who were exposed to intravenous cannulation, which predisposes catheter-associated bloodstream infections. The survey results justify the need for an antibiotic stewardship program to guide use of antibiotics.
Funding: None
Disclosures: None
If I am discussing specific healthcare products or services, I will use generic names to extent possible. If I need to use trade names, I will use trade names from several companies when available, and not just trade names from any single company.
Disagree
Christiana Kallon






